An Expert's View on Chronic Gout
PHYSICIAN VOICES
An Expert's View on Chronic Gout
By Dr. Erika Noss, MD, Ph.D.
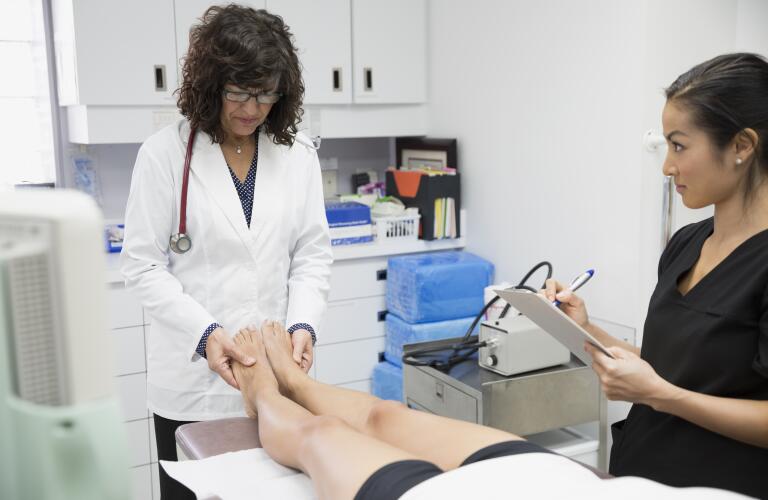
Getty
Gout stands as a chronic condition, characterized by an unpredictable cycle of acute flare-ups interspersed with periods of complete remission. While its lifelong nature might seem daunting, it is crucial to recognize that with proper management and consistent treatment, gout can be effectively controlled, significantly improving a patient's quality of life. Rheumatologist Erika Noss, MD, Ph.D., frequently addresses a core set of questions from her patients, providing valuable insights into living with and treating this complex condition. Her expertise offers a clear perspective on navigating the challenges of chronic gout, empowering individuals to manage their health proactively.
1. Q: What’s going on in the bodies of people with gout?
A: Gout manifests when there is an excessive accumulation of uric acid in the body, a condition often detected through elevated levels in blood tests. This imbalance typically stems from two primary mechanisms: either the body produces too much uric acid, or the kidneys do not efficiently eliminate enough of it. Uric acid is a natural byproduct of the metabolism of purines, compounds essential for forming DNA within our cells. Consequently, every time cells divide, become damaged, or break down, DNA is processed, leading to the creation of uric acid. This metabolic process highlights the inherent link between cellular activity and uric acid production.
What makes humans unique in this regard is a biological anomaly: primates, including humans, are the only mammals that lack a natural enzyme capable of breaking down excess uric acid. Most other mammals possess this enzyme, providing a built-in mechanism for uric acid clearance. The precise reason for this evolutionary absence in primates remains unclear, yet it directly contributes to our susceptibility to gout. Normally, the kidneys are responsible for excreting uric acid from the body. However, when uric acid levels in the bloodstream become too high, the excess can crystallize and deposit in various tissues, particularly within the joints.
When these uric acid crystals form within a joint, the immune system mistakenly identifies them as foreign invaders, triggering a robust inflammatory response. This immune attack leads to the characteristic symptoms of a gout flare: intense inflammation and severe joint pain. While younger individuals often exhibit efficient kidney function in uric acid excretion, levels can rise as people age, especially if they have pre-existing kidney disease or are overweight. In some families, gout shows a clear hereditary pattern, suggesting that genetic factors can also play a significant role in an individual's predisposition to uric acid buildup.
2. Q: Which joints does gout affect?
A: Gout flares typically begin in a highly distinctive manner, often making their first appearance in the big toe. During an initial attack, the affected toe becomes intensely red, noticeably hot to the touch, severely swollen, and excruciatingly painful, rendering walking virtually impossible. This sudden onset and extreme discomfort are hallmarks of an acute gout attack, which can be an overwhelmingly painful and explosive experience for those affected. While the big toe is the most common site for early gout symptoms, the pain is not exclusively confined there; it can also affect other joints in the foot, as well as the ankle or knees.
An immediate medical assessment for an acute gout attack is highly recommended, as prompt treatment can swiftly bring the symptoms under control. Although early attacks may eventually subside on their own without intervention, seeking professional care significantly reduces their duration and intensity. As the level of uric acid continues to accumulate in the body over time without consistent management, gout can progress, leading to the involvement of multiple joints. This chronic progression can result in the formation of visible and palpable uric acid deposits, known as nodules or tophi, which typically appear under the skin, often around affected joints or on the ears.
Left untreated, the persistent presence of uric acid crystals and recurrent inflammatory attacks can cause irreversible joint damage. This progressive destruction can lead to chronic joint pain, deformities, and significant loss of mobility, severely impacting an individual's daily life and overall function. Fortunately, such long-term and debilitating damage is largely preventable. With timely diagnosis and consistent adherence to appropriate medical treatment, the progression of gout can be halted, protecting joint health and maintaining an active lifestyle.
3. Q: What are the risk factors for developing gout?
A: Gout exhibits a clear difference in its typical onset between genders. Men are generally affected earlier in life, with the condition sometimes emerging in their 20s, though it more commonly begins in their 30s and 40s. For women, estrogen provides a protective effect against gout, making its occurrence extremely rare in those who have not yet undergone menopause. However, once menopause occurs, this hormonal protection diminishes, and women begin to develop gout at a rate comparable to men, sharing many of the same key risk factors. This shift underscores the significant role of hormonal balance in susceptibility to the condition.
Beyond gender and age, several underlying health conditions significantly increase the risk of developing gout. These include kidney disease, which impairs the body's ability to excrete uric acid effectively, leading to its accumulation. Obesity is another major factor, as it is associated with increased uric acid production and reduced excretion, often linked to insulin resistance. Furthermore, individuals with diabetes, high blood pressure, and high cholesterol also face an elevated risk, indicating a strong correlation between gout and broader metabolic health issues. Managing these co-existing conditions is therefore an integral part of comprehensive gout prevention and treatment.
Lifestyle choices also play a crucial role in the risk profile for gout. Consuming large quantities of alcohol, particularly beer, is a well-established risk factor due to its high purine content and impact on uric acid metabolism. Similarly, diets rich in red meat contribute to higher uric acid levels because of their purine density. Additionally, the regular consumption of sugary products, especially those sweetened with high-fructose corn syrup, has been linked to an increased risk of gout. These dietary components can trigger or exacerbate uric acid buildup, emphasizing the importance of mindful eating and drinking habits in managing or preventing the condition.
4. Q: How is gout treated?
A: The approach to treating gout typically involves a two-pronged strategy, designed to address both acute flare-ups and the underlying chronic condition. In the early stages of gout, when attacks are infrequent—perhaps only a few per year—medication is prescribed specifically to manage these acute episodes as they occur. This treatment is taken on an as-needed basis, providing rapid relief from the intense pain and inflammation that characterize a gout flare. The goal during this phase is to quickly subdue the symptoms and restore comfort, allowing the individual to return to their daily activities without prolonged disruption.
As the condition progresses and gout attacks become more frequent or severe, the treatment strategy shifts towards a long-term control approach. At this point, healthcare providers typically initiate a daily medication regimen designed to lower the overall levels of uric acid in the blood over time. This daily therapeutic intervention is crucial for preventing future gout flares and significantly easing persistent joint pain. By systematically reducing uric acid concentrations, these medications aim to prevent the formation of new crystals and dissolve existing ones, thereby addressing the root cause of the condition.
A critical aspect of long-term gout management is unwavering commitment to taking these prescribed medications every single day. Adherence is paramount, as inconsistent dosing, or stopping and starting the medication, dramatically increases the risk of recurrent flares. Such fluctuations in uric acid levels can provoke the immune system, leading to more frequent and intense attacks. Furthermore, if the long-term medication is not taken consistently or at all, the continuous buildup of uric acid can lead to permanent damage to the joints. Consistent daily intake is therefore not just about symptom control, but about preserving joint integrity and preventing irreversible deterioration.
5. Q: Can you manage gout with lifestyle changes?
A: While medication forms the cornerstone of effective gout management, it is equally important for patients to complement their prescribed treatment with judicious lifestyle modifications. These changes are not mere suggestions but crucial components that work in tandem with medication to help control symptoms and prevent future flares. Among the most impactful lifestyle adjustments, losing even a modest amount of weight—specifically 10 to 20 pounds—can significantly reduce uric acid levels in the body. This weight reduction can alleviate the metabolic stresses that contribute to gout, making it a highly effective and recommended intervention for many patients.
In addition to weight management, adopting a balanced diet is essential. This involves moderating the consumption of certain foods and beverages known to exacerbate gout. For instance, limiting intake of red meat and alcohol, particularly beer, is advised due to their high purine content. Furthermore, avoiding drinks sweetened with high-fructose corn syrup, such as non-diet sodas, is also recommended, as these can contribute to uric acid production. These dietary recommendations aim to minimize external sources of purines and metabolic factors that can drive uric acid elevation, thereby supporting the body’s natural mechanisms for balance.
Some individuals express a desire to manage their gout exclusively through dietary changes, hoping to eliminate the need for medication. While dietary adjustments are beneficial, attempts to achieve a completely purine-free diet have generally proven ineffective in adequately controlling uric acid levels. These extremely restrictive diets often fail to lower uric acid sufficiently to manage gout effectively, and many people find them unpalatable due to the limited food choices and lack of flavor. Therefore, a more practical and effective approach involves a combination of sensible dietary habits—such as moderate consumption of red meat, beer, and regular soda—alongside strict adherence to prescribed uric acid-lowering medication.
Original article: https://resources.healthgrades.com/right-care/gout/an-experts-view-on-chronic-gout